ARTIFICIAL CERVICAL DISC SURGERY
By:
Dr. Lali Sekhon, MBBS PhD FRACS
BACKGROUND
In technical terms, a disc in the spine is a fibrocartilaginous structure that sits between adjacent vertebral bodies. The best way to picture a disc is to imagine a tough, spongy cushion. The cushion consists of a soft inner nucleus that gives it elasticity, bounce, and recoil. A firmer outer layer provides strength and support. A key function that discs provide is they act as shock absorbers in the spine. For example, if you were to jump off a chair, about two-thirds of the load or pressure that passes through the spine would be dispersed by the discs.
When a disc ruptures, the outer part bulges and sometimes the inner nucleus escapes and can press on nerves or the spinal cord. The pressure on the nerves can cause significant pain and neurological symptoms such as numbness or tingling in the extremities the arms or legs.
If surgery is needed because of neurological symptoms, often the only way to take the pressure off the spinal cord or nerves is to entirely remove the disc. When this is done something must fill the empty space otherwise the bones keel forward and cause abnormal angling which, in themselves, may cause pain.
Most surgeons insert some form of bone into the space to fuse the vertebrae (bone) above and below the empty disc space. This often works very well in the short-term and can be done in many different ways that may include instrumentation such as cages, plates, and screws. Eventually the fusion becomes solid. There is a price to pay for such a technique. The levels above and below the fused or solid area are now forced to absorb more load as there is no spongy disc between the vertebrae. We now know that up to 30 percent of discs above or below the level of the fusion wear out within 10 years and will require surgery. A stepladder effect can occur with multiple fusions over many years.
ARTIFICIAL DISCS
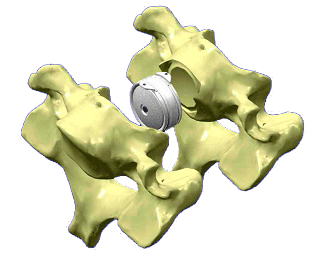
An artificial disc attempts to replace this function if the real disc has been removed. The artificial disc sits between two adjacent bones, the vertebrae, and takes the place of the original disc. An artificial disc allows movement and acts as a shock absorber. It fills the defect when a surgeon removes the disc, retains the spine’s mobility and shares the loads exerted on the spine. We hope that artificial discs also reduce the strain put onto adjacent discs, reducing the degeneration and subsequent reoperation on these discs.
There are many different types of artificial discs. They share similar design principles that include keeping the empty disc space jacked open and allowing normal spinal movement at that specific level. Some artificial discs consist of elastic polymers headed by titanium shells, such as the Bryan® disc. Others use a metal-on-metal ball and socket joint such as the Prestige® disc. In the lumbar spine, ball and socket discs are the type commonly implanted.
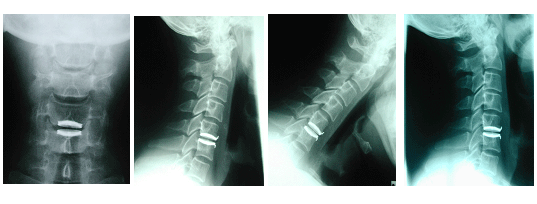
In general, cervical artificial disc replacement is used at C4-5, C5-6, and C6-7 and in the lumbar spine, L3-4, L4-5, and L5-S1. These are the levels most likely to wear out and the levels that allow most movement.
Lumbar artificial discs have been around for more than 10 years with good 10-15 year follow-up, such as the Charite® and PRODISC®. In the neck we have only had the Bryan® disc readily available for 2-3 years. Older versions have been around for over 10 years, but a lot of these have fallen out of favor.
They are available throughout the world and especially widely used in Europe and increasingly used in the Pacific Rim. In the United States, both the Bryan® disc and PRODISC are part of a current Foot and Drug Administration study. Surgeons do need specialist training in order to place these discs. In Australia, I have pioneered artificial disc surgery in the spine, performing operations on multiple levels, above fusions and reversing fusions on patients who have recently had their surgery. Early results up to 2 years are very promising.
The ideal patient for a cervical disc protrusion arthroplasty, is the same patient we would consider for an anterior cervical fusion; a patient with disc protrusion that causes arm symptoms or spinal cord compression. Ideally, only one level of the spine is replaced, but up to three levels have been done. The same patients whom we would have fused in the past are receiving artificial discs. Of course, not all patients are suitable for this technology and assessment by a skilled spinal surgeon is essential.
In the lumbar spine, the main indication for artificial disc technology is mechanical back pain with an MR showing one or two abnormal discs and a positive
discogram.
THE FUTURE IS TODAY IN SPINAL SURGERY
Artificial discs are proven in that they are safe to implant and patients are doing very well so far. The real question is what happens to these discs over time? Will they wear out? Will they need to be replaced? Lab tests up to 47 years on the Bryan® disc suggest not yet, although hip and knee replacements can wear out after 10-15 years.
The next steps are (1) a few different types will appear, all with a little difference in how they do what they do, (2) the techniques to insert them will become easier and, (3) the indications for these operations will become clarified. The era of spinal arthroplasty is definitely here.
Currently the Bryan® disc is undergoing an FDA trial in the United States. Patients with no previous surgery and single level
disease are randomized into fusions or arthroplasty. It will be 3-4 years before it is widely available in the US. Outside the U.S., in countries such as Australia, no restrictions apply and to date we have performed multilevel arthroplasties, above previous fusions and in freshly fused patients. The future is bright.
Lali
Sekhon, MBBS PhD FRACS
Royal North Shore Hospital & Dalcross Private Hospital
c/o Level 10, Citadel Tower B
799 Pacific Highway
Chatswood NSW 2067
AUSTRALIA
Tel: 61-2-94154233
Fax: 61-2-98848095
USA Fax: 909-257-8109
Email: surgeon@spinalneurosurgery.com
Website: http://www.spinalneurosurgery.com